Expert Dental Initial Claim Billing Services Across the United States
Clean Claims • Faster Payments • Stress-Free Billing
It demands work every single day to run your dental practice. Your staff is committed to providing quality service, assisting patients, and efficiently managing your practice. However, if you don't maximize your dental initial claim billing, you could be unknowingly losing money every month.
Amoha RCM is here to be your trusted partner for all your dental initial claim billing and dental claim submission requirements in the United States. We are dedicated to sending your claims out promptly and without any reductions.

What is dental initial claim billing, and why does it matter?
Dental Initial Claim Billing is the foundation of the entire process of dental billing and claim submission. This step ensures the generation and submission of claims in the right manner from the very beginning of the process. This eliminates the chances of reworks and unnecessary delays in the payment process. A clean first submission claim increases the chances of approval and accelerates the process while maintaining the health of the dental practice.
The dental claim submission process is more complex than ever, with evolving payer rules and coding updates creating multiple challenges in dental claim submission for modern practices. Incomplete and inconsistent documentation and the lack of trained professionals are some of the challenges a dental billing company faces during the process of dental claim submission. All these challenges can affect the dental practice and the process of dental claim submission in a big way.
However, if one decides to outsource the process of dental claim submission with the help of Amoha RCM, it is streamlined and efficient like never before. We use a multi-step process to ensure accuracy throughout the entire dental claim submission process. With the help of this outsourcing option, your internal team would be able to focus more on patient care and front-end operations, while we take care of the complexities involved in the billing process with utmost precision and consistency.
What Our Dental Claim Submission Services Include
At Amoha RCM, we offer dental insurance claim submission solution services to our clients, which enable them to carry out the entire billing process. Our solution is designed to bridge the gap in the process, eliminating inefficiencies so that each and every step is carried out precisely and accurately. We maintain complete control over the process from the beginning of the claim process to the end, when we post the payment.
Our Goal
"Bridging the gap in the process, eliminating inefficiencies for precision at every step."
Why Practices Rely on Amoha RCM for Dental Claim Submission
Outsourcing your dental claim submission services is a strategic move that affects your bottom line directly.
Managing your billing in-house can cost your practice anywhere from $40,000 to $70,000 a year, considering salaries, training, and turnover costs. Amoha RCM provides a more scalable and cost-effective solution with our dedicated team of experts.
Practices that outsource dental insurance claim processing experience a 15-30% increase in collections within a few months.
We also help your practice stay on top of CDT updates, HIPAA, and other payer requirements, ensuring compliance without adding extra stress to your team. Practices that invest in outsourcing dental insurance claim processing often see faster reimbursements and improved revenue cycle performance.
As your practice continues to thrive, so does our service, without adding to your hiring and training costs.
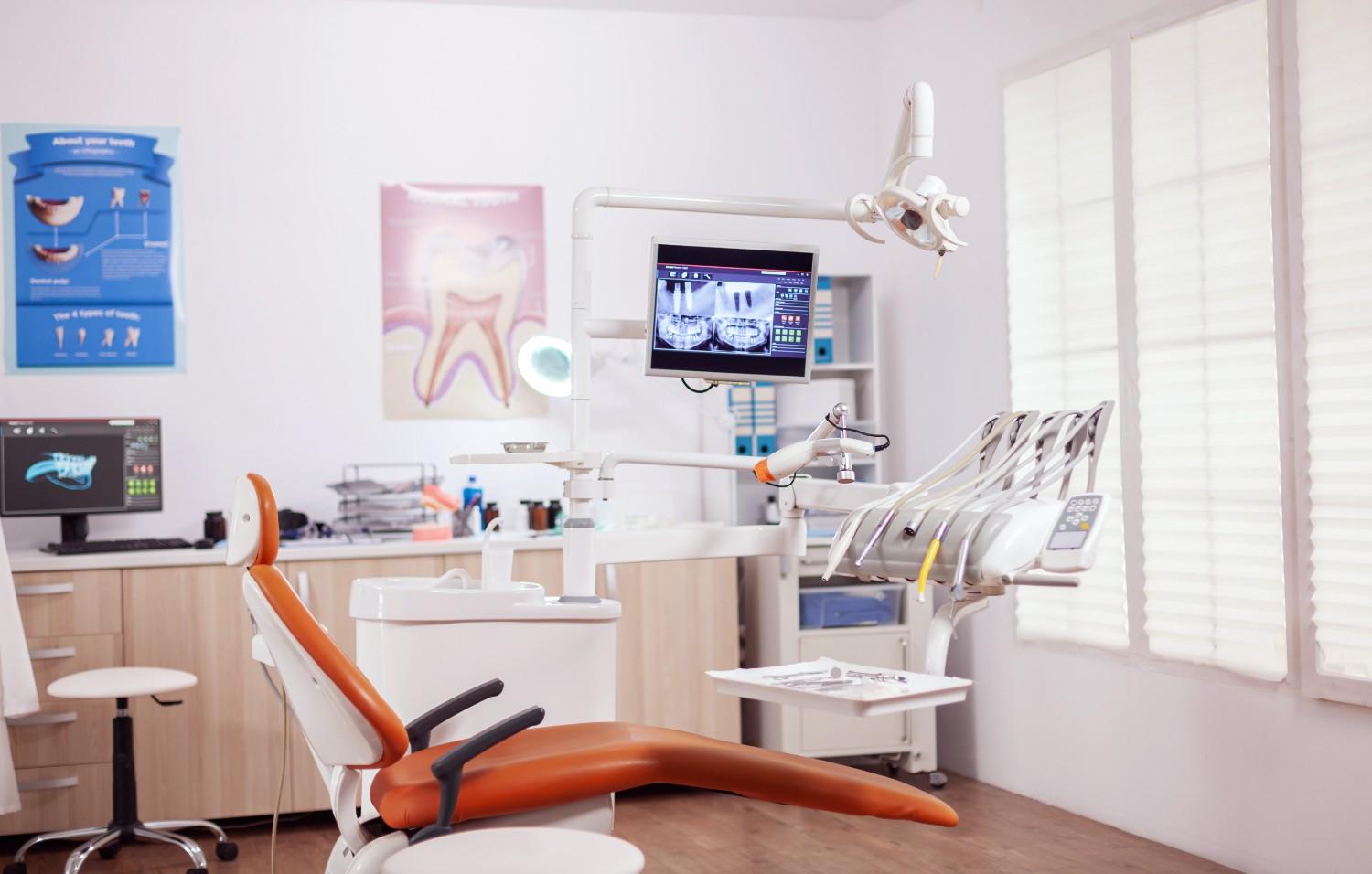
Dental Claim Submission Services for Every Specialty
Amoha RCM is known to be one of the best dental claim submission service providers. Amoha RCM works as one of the best dental claim submission companies in the USA. We serve general practices, multi-location groups, and specialists, including orthodontists, oral surgeons, periodontists, prosthodontists, and endodontists. Each of these specialties has different billing issues. Our team guarantees accurate claim submissions tailored to each specialty.
See All the Practices We ServeWhat Our Dental Claim Submission Services Include

Insurance Claim Preparation and Submission
We are experienced in handling dental initial claim billing, and we focus on accuracy and compliance in the process. Our team makes sure that each and every claim goes through an extensive review process, wherein the accuracy of CDT codes, ICD-10 codes, etc., is checked and verified, as well as whether the requirements are being met, before moving further with the claims. In addition, we ensure standardization, which reduces the scope of human errors, thereby increasing clean claims. Our team works in coordination with all the software so that your operations are not affected while we are working towards increasing backend efficiency.
Denial Management and Appeals
However, timely addressing claim denials is crucial to your practice's performance. Our team takes a thorough approach to investigating claim denials and determining the reason for them, whether it is a coding problem, a lack of documentation, or a problem related to a particular payer. We also present a compelling and well-supported appeal and resubmit claims on time to maximize your practice's revenue recovery. Further, we also look for trends in claim denials and take corrective actions to prevent such problems from happening in the future, thereby raising your claim success rate.

Insurance Eligibility Verification Solutions
We offer complete and accurate insurance eligibility verification solutions, and we do this in real time, even before a patient visits your facility. This includes coverage, benefits, co-pays, and deductibles, among other aspects. This helps prevent surprises when a patient comes to your front desk and also helps prevent denied claims due to eligibility problems. This approach helps your overall billing process from day one. We also track your denial patterns and take corrective actions to prevent similar problems from happening in the future, thereby raising your overall claim success rate.

Payment Posting and Reconciliation
Amoha RCM, a trusted provider of payment posting services, ensures the precise and accurate posting of all EOBs and ERAs. We match the payments with the claims, identify the discrepancies, and apply them accordingly. This will enable you to maintain a clean patient ledger, financial records, and practice management system with real-time data. Accurate payment posting will enable you to gain insights into your revenue cycle and make decisions accordingly. Unlike many generic payment posting companies, Amoha RCM ensures precise reconciliation aligned with your dental workflows.
Accounts Receivable Follow-Up
We closely monitor all outstanding claims and follow up on them to ensure timely reimbursement. Our staff prioritizes all outstanding claims and regularly contacts payers to address possible issues before they cause write-offs. By doing so, we help you reduce your AR days and stabilize your cash flow, keeping your revenue cycle running smoothly. We make sure no revenue is left uncollected.

Dental Credentialing Support
Our credentialing support service ensures that your healthcare providers are enrolled and credentialed with insurance payers without any delays. We take care of everything, starting from the application through to the follow-through, and then the approval. This ensures that your healthcare providers are able to start billing sooner. Hence, no loss is incurred because of a lack of credentialing. With our systematic and organized approach, we ensure that your practice is always ready to bill.
What Makes Amoha RCM Stand Out in Dental Claim Submission
What differentiates Amoha RCM from other billing and claims submission companies is its dedicated approach to dental billing and claims submission. Unlike other billing and claims submission companies, Amoha RCM is a dedicated dental billing company, and its focus helps it understand the nuances and complexities of dentistry much more.
Our dedicated account managers take the time to understand your practice, your payers, and your goals, and this process helps them communicate more effectively, work more efficiently, and develop a billing strategy that aligns with your overall revenue goals. This focused approach is what makes us one of the best dental claim submission services for practices across the United States.
Our real-time dashboards provide you with complete transparency into your claims, denials, collections, and accounts receivable status, and our easy-to-understand reports help you stay up to date on your overall revenue status.
Dedicated Dental Billing Company
Unlike other billing and claims submission companies, Amoha RCM is a dedicated dental billing company, and its focus helps it understand the nuances and complexities of dentistry much more.
Dedicated Account Managers
Our dedicated account managers take the time to understand your practice, your payers, and your goals, developing a billing strategy that aligns with your overall revenue goals.
Real-Time Dashboards
Our real-time dashboards provide you with complete transparency into your claims, denials, collections, and accounts receivable status.
Easy-to-Understand Reports
Our easy-to-understand reports help you stay up to date on your overall revenue status - no finance degree required.
15-30% Collections Increase
Practices that outsource dental insurance claim processing experience a 15-30% increase in collections within a few months.
CDT & HIPAA Compliance
We help your practice stay on top of CDT updates, HIPAA, and other payer requirements, ensuring compliance without adding extra stress to your team.
Ready to Improve Your Dental Initial Claim Billing Process?
Your practice works hard to make every dollar count. Your practice deserves a system that efficiently collects every hard-earned dollar. No more lost revenue because of claim errors and delays. Unite with Amoha RCM and take advantage of the best in dental insurance claim submission services.
Frequently Asked Questions
Our dental claim submission service involves all aspects of claims, including claim preparation, coding, timely submission, real-time eligibility, payment, and accounts receivable follow-up. We guarantee precision in all aspects of our work, ensuring your practice receives optimal reimbursement with minimal delays.
